Breast cancer screening — deciding what's best for you

It’s Breast Cancer Awareness month and everywhere we turn there are pink ribbons, as well as news stories reporting as much (or more) misinformation as helpful. Based on sometimes alarming media portrayals, breast cancer is afflicting growing numbers of women. Few women will make it to Halloween without feeling anxious and worried that they’ll be next.
Of course, we all want to support the best clinical research and nail these cancers with the most effective treatments that will save women’s lives. But it’s also easy to get behind anything that sounds beneficial, believing better-safe-than-sorry is always best. Screening is one such intervention that seems like a slam dunk. After all, “what could be the harm?”
But, as the medical literature has explored, cancer screening is more complicated than 'early detection means better survival'. With any health intervention — even something as intuitively simple as promoting healthy eating and exercise to children — there are always risks and potential harms that have to be weighed against the strength of the evidence of their benefits.
It can be exceedingly hard, though, for women to find information exploring the pros and cons of screenings — or to even learn that there are two sides to the issue — when making decisions as to what’s best for them. The Daily Mail took a unique step to publish an interesting point-counterpoint article between two medical experts to respond to the question: “Does breast cancer screening do more harm than good?”
Reporter Thea Jourdan opened by noting that breast cancer is seen as a medical success story, with 8 out of every ten women surviving beyond five years, compared to just half of women diagnosed just 30 years ago. Many credit breast cancer screening with saving lives, she writes, while others say that screening has increased the number of women diagnosed as cancer victims for small latent cancers that would never have amounted to much and exaggerated the seemingly improved survival rates, while also causing undue anxiety and unnecessary medical interventions.
YES
 Arguing “Yes” that breast cancer screening does more harm than good was Dr. Michael Baum, Emeritus Professor of Surgery and visiting professor of Medical Humanities at University College, London. A British oncologist, specializing in breast cancer treatment for 40 years, Dr. Baum has also led research on breast-conserving surgery and tamoxifen, and authored Breast Cancer Fast Facts. He writes:
Arguing “Yes” that breast cancer screening does more harm than good was Dr. Michael Baum, Emeritus Professor of Surgery and visiting professor of Medical Humanities at University College, London. A British oncologist, specializing in breast cancer treatment for 40 years, Dr. Baum has also led research on breast-conserving surgery and tamoxifen, and authored Breast Cancer Fast Facts. He writes:
Each year I dread Breast Cancer Awareness month — I've christened it 'Black October', because all it does is scare women. It creates a disproportionate number of worried women who become overly anxious about their health, without any evidence that this greater awareness contributes to a drop in breast cancer mortality. I also have grave doubts about the screening programme. It, too, causes far more problems than it solves and I speak as someone who was initially enthusiastic about it, setting up the first breast screening centre in south-east England in 1987… But the more I learned, the more sceptical I became.
It misdiagnosed many women, and it didn't catch many aggressive tumours. I also noticed that women were becoming more anxious about the spectre of 'breast cancer' than they needed to be… In 1997, I resigned from the national screening committee over the issue of consent. I didn't believe women were being given a fair or informed choice, because they were not getting all the facts about the failings of the screening programme.
Dr. Baum then explains why he objects so strongly, writing:
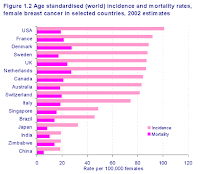 First, it has created a false impression that we are in the grip of a breast cancer epidemic. Interestingly, every country that introduces a screening programme has an overnight leap in breast cancer incidence. [Figure from Cancer Research UK.] This isn't because many cases of cancer were previously going undetected, but because screenings pick up latent cancers and anomalies that would not cause any problems if left alone.
First, it has created a false impression that we are in the grip of a breast cancer epidemic. Interestingly, every country that introduces a screening programme has an overnight leap in breast cancer incidence. [Figure from Cancer Research UK.] This isn't because many cases of cancer were previously going undetected, but because screenings pick up latent cancers and anomalies that would not cause any problems if left alone.
According to the Cochrane Collaboration, a research organisation, between 20 and 50 percent of screening-detected cancers are 'over-diagnosed'. Put simply, at least a quarter of women who are told they have breast cancer would have died from other causes if the cancer had not been detected.
Yet because of their 'diagnosis', these women undergo invasive procedures — such as biopsy — and suffer unnecessary misery. After the biopsy, the pathologist's report may reveal borderline abnormalities — these are unlikely to lead to cancer, yet fear of litigation means this cannot be ignored. So the women often undergo surgery to remove the 'cancer' that, left alone, may never have caused harm…
Dr. Baum goes on to discuss the flawed statistics that appear to show early diagnosis through screening leads to less invasive procedures and that screening programs save lives. His side of the issue is so rarely mentioned, few women may even be aware there is a downside to screening, and his next statement may come as the greatest surprise. He adds:
The fact is that the screening programme is not even effective at saving lives. Screening takes place every three years, so it doesn't tend to catch the fast-growing, aggressive cancers, such as high-grade invasive duct carcinoma and inflammatory breast cancer [ the ones especially imperative to treat]. Furthermore, only one in 1,000 women will avoid death from breast cancer over ten years of attending screening. Yes, that one life is of infinite value, but think of the downside for all the anxious misdiagnosed women who suffer.
Instead of the screening establishment making decisions on behalf of women, surely women should be given all the facts to make their own decisions. To believe otherwise is patronising.
As for the decline in the death rate in the past 20 years, I don't think this has anything to do with the screening programme, as this drop is also seen in younger women who are not invited for routine screening. The difference has been better education and treatments, including more effective drug therapies. The NHS breast screening programme has an annual budget of around £75 million - imagine what we could achieve if that money was spent instead on research into prevention and cure.
NO
Arguing “No” that breast cancer screening does not do more harm than good was Dr. Michael Michell, a consultant radiologist at King's College Hospital and the director of the South East London Breast Screening Programme. He has worked with breast cancer patients for 25 years, according to Ms. Jourdan. Dr. Mitchell writes:
I know it saves lives. Over the past 20 years, the programme has screened 19 million women and has saved at least 25,000 women from a premature death from breast cancer. When I started working in Breast Clinics at King's College Hospital in the Eighties, it was common to see women who had aggressive cancer where the tumour was eroding the skin. Now, we rarely see such cases because of better public awareness of the disease and because the screening programme has detected many small cancers before they have progressed.
Yes, screenings may cause some women extra anxiety, but it reassures a lot more women that they are taking control of their own health. There is strong evidence from trials that screenings are very effective at picking up cancers when they are small and easy to treat. Just using fingertip-examination alone is not a good way to find early-stage cancers. If we find them, we can treat them… It's true that any screening programme will pick up some cancers which won't go on to be life-threatening. But if I was a woman, I would not want to take that risk…
Dr. Michell continues by addressing women's fears of breast cancer treatment, adding:
And mastectomy is not as devastating as it once was. Modern plastic surgery techniques ensure that an excellent cosmetic result can be obtained after surgery to restore the shape of the breast. Women should be able to end up with a normal breast contour, or sometimes even an enhanced breast contour. And women do have the information they need to make an informed choice.
Every woman invited for screening receives a booklet which outlines the pros and cons. At the end of the day, it is their decision to go ahead and have a mammogram. Sadly, we know that the rate of breast cancer has been increasing. It's been rising since long before the screening programme was implemented, and it goes across the age groups. So screening is actually one of our best weapons in defence against deaths from breast cancer and, of course, it should continue… Three-quarters of women who receive an invitation for screening, come and have their breasts checked out. That's a good enough endorsement for me.
Some stats
Anytime people are frightened and believe they’re in the midst of a health epidemic or at heightened risk, the sense of urgency to act is increased. For American readers, however, our government’s best data shows no epidemic of breast cancer. The Centers for Disease Control and Prevention report on the incidence of breast cancers among women in the U.S. was published last summer in the MMWR Weekly. Researchers with the Division of Cancer Prevention and Control said that data from the National Cancer Institute’s Surveillance, Epidemiology and End Results (SEER) program and from the CDC’s National Program of Cancer Registries (NPCR) together indicate that:
For American readers, however, our government’s best data shows no epidemic of breast cancer. The Centers for Disease Control and Prevention report on the incidence of breast cancers among women in the U.S. was published last summer in the MMWR Weekly. Researchers with the Division of Cancer Prevention and Control said that data from the National Cancer Institute’s Surveillance, Epidemiology and End Results (SEER) program and from the CDC’s National Program of Cancer Registries (NPCR) together indicate that:
[A]ge-adjusted incidence rates for invasive breast cancer decreased each year during 1999-2003, with the greatest decrease (6.1%) occurring from 2002 to 2003; women aged >50 years experienced a significant decrease during this period. Rates of in-situ (noninvasive) breast cancer increased each year during 1999-2002 and then decreased from 2002 to 2003; women aged 50-79 years experienced a significant decrease during this period.
 Breast cancer mortality rates have also shown declines, according to the CDC, dropping 2.3% per year throughout 1990 to 2000. Breast cancer deaths in the UK, have also fallen, by one-third since the late 1980s, according to Cancer Research UK.
Breast cancer mortality rates have also shown declines, according to the CDC, dropping 2.3% per year throughout 1990 to 2000. Breast cancer deaths in the UK, have also fallen, by one-third since the late 1980s, according to Cancer Research UK.
Concerning Dr. Baum’s comments on screenings’ effect on reported incident rates, the CDC editors described research analyzing all breast cancer incidence rates throughout 1943-2002 which had generally “indicated that although incidence rates increased over time, they increased more quickly after initiation of mammography screening recommendations in the early 1980s, suggesting that more cases were being detected through screening.”
Like many cancers, the risks of being diagnosed with, as well as dying from, an invasive breast cancer rise with age. The actual incidence rates, though, may be less than what many women may fear. Between 1999-2003, about 0.012% of young women through age 30 were diagnosed with an invasive breast cancer. Incidence rates were 0.145% for women in their 40s; 0.25% for women in their 50s; 0.35% for women in their 60s; 0.4% among women in their 70s and finally, 0.37% among women in their 80s.
According to SEER-NCHS data, the probability a woman will develop any type of breast cancer between age 50 to 70 is 5.62% — and 94.38% chance she won’t.
Reviews of the evidence and informed consent?
Do American women hear all sides of breast screening, understand false positives and negatives and the potential adverse outcomes, and feel free to make their own informed decisions? Most often, news stories present mammographies and even MRIs as indispensable for women who want to be certain they’re doing everything they can to lower their risk of dying from breast cancer.
In contrast to media reports, objective reviews of the evidence to date present less decisive benefits. The Cochrane Collaborative’s Systemic Review of mammograms mentioned by Dr. Baum was covered here. Bottom line, after examining the highest quality, randomized trials involving half a million women, it reported that even after 13 years of follow-up, no reduction in breast cancer mortality was seen in those studies.
An earlier 2002 Summary of the Evidence by the U.S. Preventive Services Task Force found the evidence fair that routine mammography reduces mortality from breast cancer. The probability of benefit increase with advancing age from 50 to 70 years; while the likelihood of harms from screening (false-positive results and unnecessary anxiety, biopsies, and cost) increase with lowering ages. “The precise age at which the potential benefits of mammography justify the possible harms is a subjective choice,” it concluded. “Mammography sensitivity ranges between 77% and 95% and specificity between 94% and 97%.” But both sensitivity and specificity are lower with younger women and those with more dense breasts, according to its Evidence Summary.
The research shows that 12% to 78% of mammograms require subsequent biopsies, according to the USPSTF. The number needed to screen to prevent one breast cancer death after about 14 years of follow-up is 1,792 among women under age 50; 1,224 among women in all age groups; and 838 among women aged 50 to 74.” It went on to offer B-level Recommendation for mammography for women aged 40 and over.
American women get mammograms when ‘invited to’ at about the same rate as Dr. Michell reported in England, with a national average of about 72%. Routine breast mammography screenings for all women have become part of HEDIS measures, the performance measure mandated by more than 90% of the nation’s health plans, meaning, both medical providers and health plan members are encouraged to abide by them. Providers are also graded via Quality Score Cards, for example, based on their compliance with these performance measures. Yet, member information from most health plans talks only of the benefits of mammography and makes no mention of downsides.
Kaiser Permanente in Southern California has the highest breast cancer screening rate for women aged 52 to 69 in the nation — with over 87% of women getting their recommended mammograms. In describing the techniques it has used to reach this compliance rate, executive medical director, Dr. Jeffrey Weisz, M.D., told Market Watch:
"We have made it our mission to reach out to every woman between the ages of 52 to 69, reminding them, coaxing them, and making it easy for them to get their mammograms." Kaiser Permanente's electronic medical record system, KP HealthConnect, flags the file of each woman who is due for a mammogram. When the record comes up at any visit, the check-in receptionist, nurse, or physician, even those in orthopedics, ophthalmology, or any specialty, will remind the patient that walk-in mammograms are available. Whether it was for an injured ankle or an eye exam, after the original visit, the patient can make a future mammogram appointment or go immediately to get a mammogram. For those who put off their breast cancer screening, or never come for a visit, there are follow-up letters, reminders, and personal phone calls.
There was no mention of any potential downsides of screening in that story. Gary Schwitzer at the University of Minnesota School of Journalism & Mass Communication, noted another news story which failed to provide balance. He took issue last Friday with CBS Early Show for promoting self-breast examinations, featuring Olivia Newton-John’s Liv Aid kit. The show was veritable commercial air time and made no mention of the latest review of the scientific literature, he said. It provided “one-sided, incomplete information to its viewers.”
Both major objective reviews of the clinical trial evidence on breast examinations, whether by women themselves or done by a healthcare professional, have found no support of a benefit. As the Cochrane Collaboration review of randomized clinical trials involving 388,535 women, concluded this year:
The review of data from these trials did not find a beneficial effect of screening in terms of improvement in breast cancer mortality. The trials showed that women who were randomised to breast self-examination were almost twice as likely to undergo a biopsy of the breast, with 3406 biopsies performed in the screening group compared to 1856 biopsies in the control group…
Data from two large trials do not suggest a beneficial effect of screening by breast self-examination but do suggest increased harm in terms of increased numbers of benign lesions identified and an increased number of biopsies performed. At present, screening by breast self-examination or physical examination cannot be recommended.
These findings concur with the earlier U.S. Preventive Services Task Force Summary of the Evidence published in 2002, which concluded “the evidence is insufficient to recommend for or against routine clinical breast examination alone to screen for breast cancer…Breast self-examination has not been shown to reduce breast cancer mortality in the best studies to date.”
Informed consent — National Cancer Institute
In contrast to patient information from health plans and media, that from the National Cancer Institute does include information on the Risks of Breast Cancer Screening for women to consider in order to make a truly informed consent and decide what may be best for them, as mentioned by Dr. Baum. The NCI states:
Screening tests have risks.
Decisions about screening tests can be difficult. Not all screening tests are helpful and most have risks. Before having any screening test, you may want to discuss the test with your doctor. It is important to know the risks of the test and whether it has been proven to reduce the risk of dying from cancer.
The risks of breast cancer screening tests include the following:
Finding breast cancer may not improve health or help a woman live longer.
Screening may not help you if you have fast-growing breast cancer or if it has already spread to other places in your body. Also, some breast cancers found on a screening mammogram may never cause symptoms or become life-threatening. When such cancers are found, treatment would not help you live longer and may instead cause serious treatment-related side effects. At this time, it is not possible to be sure which breast cancers found by screening will cause symptoms and which breast cancers will not.
False-negative test results can occur.
Screening test results may appear to be normal even though breast cancer is present. A woman who receives a false-negative test result (one that shows there is no cancer when there really is) may delay seeking medical care even if she has symptoms.
One in 5 cancers may be missed by mammography. False-negatives occur more often in younger women than in older women because the breast tissue of younger women is more dense. The size of the tumor, the rate of tumor growth, the level of hormones, such as estrogen and progesterone, in the woman’s body, and the skill of the radiologist can also affect the chance of a false-negative result.
False-positive test results can occur.
Screening test results may appear to be abnormal even though no cancer is present. A false-positive test result (one that shows there is cancer when there really isn’t) can cause anxiety and is usually followed by more tests (such as biopsy), which also have risks.
Most abnormal test results turn out not to be cancer. False-positives are more common in younger women, women who have had previous breast biopsies, women with a family history of breast cancer, and women who take hormones, such as estrogen and progesterone. The skill of the doctor also can affect the chance of a false-positive result.
Mammograms expose the breast to radiation.
Being exposed to radiation is a risk factor for breast cancer. The risk of developing breast cancer from radiation exposure, such as screening mammograms or x-rays, is greater with higher doses of radiation and in younger women. For women older than 40 years, the benefits of an annual screening mammogram may be greater than the risks from radiation exposure.
The risks and benefits of screening for breast cancer may be different for different groups of people.
The benefits of breast cancer screening may vary among age groups:
● In women who have a life expectancy of 5 years or less, finding and treating early stage breast cancer may reduce their quality of life without helping them live longer.
● In women older than 65 years, the results of a screening test may lead to more diagnostic tests and anxiety while waiting for the test results. Also, the breast cancers found are usually not life-threatening.
● In women 35 years or younger who go to the doctor for breast symptoms, mammogram results may not be helpful in managing their care.
Routine breast cancer screening is advised for women who have had radiation treatment to the chest, especially at a young age. The benefits and risks of mammograms and MRIs for these women are not known. There is no information on the benefits or risks of breast cancer screening in men.
No matter how old you are, if you have risk factors for breast cancer you should ask for medical advice about when to begin having mammograms and how often to be screened.
Regardless of your screening decision, anyone who discovers any unusual lumps, thickening, nipple discharge or breast changes of any kind, should see their doctor. While a lot of preventive health screenings are controversial, there is no controversy about getting prompt medical care for actual symptoms.
When making a decision about breast cancer screening or any medical procedure, the answers aren’t always intuitive or simple. In order to make an informed choice, every woman deserves to know all sides and feel free to decide what’s best for her. That’s real breast cancer awareness.
© 2008 Sandy Szwarc




<< Home