Paradoxes compel us to think — Part Two

Paradoxes Part One here.
Continuing with paradoxical correlations recently published in medical journals that we didn’t hear about, comes an analysis of the Helsinki Businessmen Study. As the authors noted, ‘obese’ or ‘overweight’ is associated in the medical literature with a better prognosis and lower death rates compared with ‘normal’ weight people, especially as people get older. They set out to see if losing or gaining weight during one’s adult life, or if traditional cardiac risk factors in middle-age, could potentially explain the obesity paradox. The authors reported finding that being overweight or losing weight in midlife had the worst prognosis and greatest risk of dying later in life.
Did you catch what they didn’t say?
Who had the best prognosis and lowest mortality risk? Those who gained weight and became fat.
This study offers some valuable take-home lessons, such as the importance for us to examine what a study’s data actually showed, to understand correlations and to read critically to get the full story.
Overview
Briefly, the Helsinki Businessmen Study cohort offered a valuable opportunity to test the obesity paradox because the men were similar in social and economic status, age, healthcare access and other factors that confound health and mortality outcomes. They were all healthy business executives who had participated in comprehensive medical check-ups during the 1960s and early 1970s at the Institute of Occupational Health in Helsinki. The study database had information on their BMIs and cardiovascular risk factors at multiple times during their lives, from the age of 25 through an average age of 73 years. The men who survived to the year 2000 were surveyed again to determine their BMI and health, and although self-reported, these health surveys had been validated in the Finnish population. The few men lost in follow-up were not different from the rest of the men by any measure examined. Mortality data was known on all the men because Finnish citizens are registered with the Population Information System, which keeps health and cause of death information.
The authors, led by Professor Timo Strandberg at the Institute of Health Sciences/Geriatrics at the University of Oulu, Finland, set out to explain the obesity paradox. They divided the men into those whose BMIs had remained in the ‘normal’ weight range and those who were fat (BMI >25) at each point in their lives that they’d been recorded, those who had been normal weight in 1974 but became fat later in life, and those who’d been fat in 1974 but lost weight and achieved a normal weight. Their results were published in the European Heart Journal.
How well did the traditional cardiac risk factors — health indices that included BMI, blood lipids (cholesterol), blood glucose and blood pressure; smoking habits and exercise — actually predict mortality and those men who went on to develop chronic diseases? Not surprising to regular JFS readers, regardless of the traditional cardiac risk factors, there was no statistical difference among those who went on to develop coronary heart disease, peripheral artery disease, cancer, pulmonary disease or dementia.
The only statistically significant inverse correlations to the men’s BMIs were with diabetes and hypertension — but they didn’t affect the men’s mortality rates, perhaps because, as we’ve seen, heavier people with both conditions have lower health complications compared to slender people with those conditions. Other popular myths weren’t supported in this study, which also won’t surprise regular readers who’ve followed the research. The men who gained weight as they aged and those who lost weight to achieve a normal weight had identical rates of developing diabetes, and the same cholesterol levels and blood pressures, as they aged.
Consistently overweight men made up the largest group of men who survived to the year 2000 (44% versus 30% of those who’d maintained normal weights). And, despite reports that the consistently overweight men had the worst prognosis, in follow-up through 2006, they actually had no statistical difference in mortality (HR=1.1 with confidence level 0.7-1.6) compared to the naturally normal weight men (HR=1.0).
But by every statistical analysis the authors attempted — including adjusting for potential confounding factors that included age, smoking status, and chronic diseases of aging (cancer, diabetes, dementia, cerebrovascular disorders, heart disease and heart failure, pulmonary disease, musculoskeletal disease and hypertension) — the men who’d been overweight but lost weight during middle adulthood to reach normal weights had about two times the risk of death compared to normal weight men or the men who’d just stayed fat. The risks steadily rose regardless of the years followed through 2006.

In comparison, the men who had gained weight during adulthood (gaining an average of 17.6 pounds from age 25, with about 15 pounds gained during middle age from around age 47) had the lowest mortality rates: 30 percent lower than the men who’d maintained normal or overweight status. While this hazard ratio isn’t tenable, as we know, gaining weight with age certainly isn’t the death sentence popularly believed.
Beliefs in the deadliness of weight gain and “middle-age spread,” and beliefs in the health benefits of watching your weight and losing weight, were not supported in this study. Even the authors appeared to struggle to interpret their own findings. These seeming paradoxes, though, weren’t paradoxes to obesity researchers. But decades of medical research which contradicts these popularized beliefs rarely reaches the public and their value as null studies was lost. Looking at just a few of those studies may give you an idea of how much inconvenient research never finds its way to consumers.
Mortality and weight loss
Beliefs about weight loss have become so widespread, few people stop to question if its benefits have ever been proven or, worse, if it could place people at greater risks for harm. Yet the potential health dangers of voluntary weight loss have been recognized among medical researchers for decades.
It goes beyond the recognized failures and side effects of weight loss prescriptions in nutritional shortfalls; diminished concentration, mental acuity, learning and productivity; cardiac arrhythmias; osteoporosis; heightened stigma of fat people; and eating disorders. The physiological and emotional changes that occur with chronic food restriction and restrained eating, as in eating disorders, for example, are similar to those experienced by starving people but are seldom understood as symptoms of hunger. The side effects of weight loss efforts, especially those begun at young ages, go beyond the effects on people’s lives, teaching generations to fear and have dysfunctional relationships with food and their natural bodies and appetites until many don’t know what normal eating is anymore.
 The risks are downplayed and perceived to be warranted because, it’s believed, weight loss and maintaining normal weight is achievable and reduces mortality and prevents chronic diseases of aging — despite the fact that even the U.S. Preventive Services Task Force found little credible support for weight loss as having positive effects on overall mortality, mental health or daily functioning.
The risks are downplayed and perceived to be warranted because, it’s believed, weight loss and maintaining normal weight is achievable and reduces mortality and prevents chronic diseases of aging — despite the fact that even the U.S. Preventive Services Task Force found little credible support for weight loss as having positive effects on overall mortality, mental health or daily functioning.
In 1992, the National Institutes of Health held what is still the most pivotal conference on Methods for Voluntary Weight Loss and Control, when experts reviewed nearly half a century of evidence on voluntary weight loss. It found that most studies, and the strongest evidence, showed voluntary weight loss regardless of the method, although seemingly to reduce risk factors, was strongly associated with increased rates of actual clinical outcomes including heart disease, stroke, type 2 diabetes and cancers, as well as increased rates for premature death — by as much as several hundred percent in some studies.
Time and again in randomized clinical trials of pharmaceuticals and other medical interventions, we’ve seen the importance of examining confirmed clinical endpoints — with all-cause mortality the most important — rather than surrogate endpoints. Not understanding risk factors and believing that these surrogate health indices are measures of health and future disease has been the greatest way the public been led to believe that weight loss is beneficial, even when it’s not supported in well controlled studies looking at actual clinical outcomes and mortality. With fasting, starvation/dieting and weight loss, most indices (blood sugar, cholesterol, blood pressure, weight, etc) temporarily drop and can be used to claim the short-term health benefits of dieting and weight loss — before they rebound, often to higher levels over the long-term.
 German epidemiologists, examining 13,362 middle-aged adult men and women in the European Prospective Investigation into Cancer and Nutrition-Potsdam Study, for example, found that fat people who had normal blood pressures prior to weight loss had a nearly 7-fold increased risk of developing essential hypertension during the following two years after weight loss, and those whose weight yo-yoed had a 4.29-fold increase in hypertension.
German epidemiologists, examining 13,362 middle-aged adult men and women in the European Prospective Investigation into Cancer and Nutrition-Potsdam Study, for example, found that fat people who had normal blood pressures prior to weight loss had a nearly 7-fold increased risk of developing essential hypertension during the following two years after weight loss, and those whose weight yo-yoed had a 4.29-fold increase in hypertension.
Dr. Reubin Andres, M.D., a gerontologist at the National Institute on Aging and a professor of medicine at Johns Hopkins, admitted that weight loss can improve blood sugar levels, blood pressure and cholesterol in the short term. “The only problem is that when you look at mortality rates,” he said, “they don’t look good. Fat people who are subject to weight loss have a higher mortality rate than those who remain fat.”
In a later review published in a 1993 issue of the Annals of Internal Medicine, Dr. Andres and colleagues summarized the findings of 13 international studies on prolonged voluntary weight loss and mortality among adults who had been followed for eight or more years. The studies they included had made every effort to eliminate potential confounding influences of involuntary weight loss, which is generally seen as an important symptom of serious illness. For example, clinical exams were conducted at the end of weight loss to identify and exclude those with identifiable illnesses. They also applied a “temporal separation” period, excluding several years at the beginning of their analysis to eliminate people who may have had undetected illness at the time of enrollment. Ten of the 13 studies had factored for the effects of smoking, which is commonly associated with both lower weight and higher mortality. They noted, however, that: “Studies that have accounted for smoking habits have generally failed to show any significant effects of smoking on the association between weight change and death.”
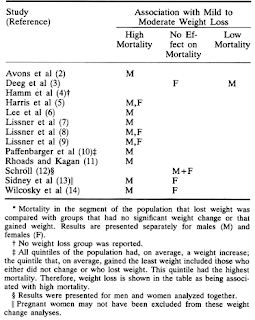
The predominance of the research they examined showed that modest to moderate weight loss is associated with high mortality compared to those with no significant weight change or who gained weight. [The only study which hadn’t found high mortality was the Dutch Longitudinal Study (Deeg etal), conducted between 1955 and 1957. It was the smallest and had only reported longevity in terms of probabilities and found no statistically significant.] The preponderance of studies, eleven in all, found weight gain was associated with the lowest all-cause mortality.
Dr. Andres and colleagues concluded:
The current analysis of 13 studies of weight change now provides support for the concept that some degree of weight gain during adulthood is associated with lower all-cause mortality rates. The results of these analyses show that persons who gain some weight during adulthood survive longer, on average, than do those who maintain or lose weight and that long-term weight loss, even of a mild or moderate degree, is generally associated with high mortality rate.
The later Cardiovascular Health Study was a longitudinal observational study of 4,714 seniors, aged 65 years and older, sponsored by the National Heart, Lung, and Blood Institute. Participants were recruited from random samples of Medicare eligibility lists in four U.S. communities and their weights were measured at least five times between 1992 and 1999. The authors assessed the effects of weight change on mortality over another seven years of follow-up. After adjusting for confounding factors, such as illnesses, cancer, diabetes and overall health status, age, smoking, hospitalization, education, death of a spouse, disability, strength and gait speed, they found that even modest weight loss of just 5 percent or more was associated with an 82 percent higher risk of mortality, with those who were the slimmest at the beginning of the study had the highest mortality. Those whose weights yo-yoed were associated with a 2.2-fold higher risk for death compared to those with stable weights or who gained weight.
Studies have found similar results among adults of all ages. A study examining mortality among a nationally representative sample of the United States population — people who had had their weights measured as part of NHANES I — for example, failed to support the benefits of weight loss for fat people. Even after controlling for pre-existing disease, health and disability, weight fluctuations were associated with an 83 percent higher mortality risk. Among those who lost weight, mortality was 3.36-fold higher compared with those who stayed obese.
Obesity researchers have been questioning the long-term benefits on weight loss in the medical literature for decades, but these discussions — along with the null and negative studies — seldom get through the weight loss marketing to reach the general public. For example, in a 1999 issue of the International Journal of Obesity, Dr. Thorkild Sorensen with the Danish Epidemiological Science Centre at the Institute of Preventive Medicine in Copenhagen, Denmark, argued that sustained weight loss may not lead to decreased mortality and morbidity. Dr. Sorensen noted that major risk factors improve immediately during weight loss, but said that the reason to doubt the long-term benefits of weight loss is that “several epidemiological studies have been unable to demonstrate that long-term weight loss is followed by reduced mortality.” “To the contrary,” he said, “some studies suggest that weight loss is associated with increased mortality relative to the mortality associated with stable weight, and even that associated with stable overweight.”
The tempting explanation to explain away these findings has been that diseases associated with increased mortality cause unintentional weight loss. Another frequently proposed assertion is that those who lose weight have taken up adverse lifestyles, such as smoking or drinking. “However, in very carefully controlled population-based prospective studies, in which smoking, as well we preexisting and incident diseases, is taken into account, an increased mortality associated with weight loss remains,” he said. “Meta-analysis of long term results of weight loss indicate that after five years about 97 percent of subjects losing weight have regained that weight or even exceeded pre-treatment levels.”
 It’s been argued, he summarized, that weight loss does not equal improvement in health and longevity, that staying fat is safer than weight fluctuations, and dieting has negative psychological effects. “In summary, we still do not have conclusive evidence that weight loss has overall beneficial effects.”
It’s been argued, he summarized, that weight loss does not equal improvement in health and longevity, that staying fat is safer than weight fluctuations, and dieting has negative psychological effects. “In summary, we still do not have conclusive evidence that weight loss has overall beneficial effects.”
These researchers at the Danish Epidemiology Science Centre also investigated the effects on mortality of intentional weight loss alone. They examined mortality of nearly 3,000 fat people without pre-existing or current diseases who reported they had been trying to lose weight. The authors even controlled for behavioral and psychological risk factors and hypertension as potential confounding factors. Interestingly, those who were successful at weight loss had 86 percent increased risks of mortality compared to those who weren’t trying to lose weight and whose weight remained stable. While those who gained weight were associated with a 7 percent lower risk of mortality. Unintentional changes in weight — regardless of down and up, (which is rarely recognized as a symptom of disease rather than lifestyle) — were associated with higher risks. While none of the correlations were tenable or proof of causation, they did lead the authors to conclude that “deliberate weight loss in overweight individuals without known co-morbidities may be hazardous in the long term.”
Another valuable aspect of the study by Dr. Strandberg and colleagues was that it examined a group of men of similar occupational and economic status. Carefully controlled studies try to account for known influences on health and mortality — such as age and pre-existing disease. Epidemiological studies that claim to find associations between weight changes and mortality often poorly control for social class and economic status. Yet social standing and economic status have each been independently found to be strongly tied with health disparities. As regular JFS readers have seen, for instance, people living in socially disadvantaged settings and who experience social stigma have significantly higher rates of heart disease, diabetes and premature deaths compared to middle-incomes, even controlling for age, education, gender, healthcare access, cardiac risk factors (smoking, weight, blood pressure, blood cholesterol levels, etc.), diets and lifestyles .
Weight gain can be a marker of lower social class and economic status, yet weight is then inappropriately blamed for the poorer health and mortality. Popular beliefs and prejudices lead many to assume that poor people must be eating more, not be as physically active or eating unhealthy foods to explain their higher weight gains and mortality. But these prejudicial beliefs have not held up in the scientific literature.
A study of the European Prospective Investigation into Cancer and Nutrition—Norfolk cohort, for example, looked at data from medical examinations and lifestyle assessments that had been done on 14,619 healthy adults in 1993-7 and again during 1998-2000. People in low socioeconomic status gained more weight during middle-age — but the weight changes were unrelated to the calories they consumed or their activity levels, even after controlling for other traditional obesity risk factors.
 Classism and prejudices have popularized beliefs, even among fat people, that lower-income people don’t know how to eat properly or how to feed their children and are eating mostly junk. If they ate “right” — i.e. more fresh fruits and vegetables — they would be healthier (and thinner), so the thinking goes. Besides the fact that the body of evidence consistently shows that fat and thin eat no differently to explain the diversities of their sizes, income doesn’t explain the diversities of their nutritional status, either. Population dietary studies published for well over 50 years have shown that in developed countries, low income children and families don’t eat appreciably different nutrients from higher income families.
Classism and prejudices have popularized beliefs, even among fat people, that lower-income people don’t know how to eat properly or how to feed their children and are eating mostly junk. If they ate “right” — i.e. more fresh fruits and vegetables — they would be healthier (and thinner), so the thinking goes. Besides the fact that the body of evidence consistently shows that fat and thin eat no differently to explain the diversities of their sizes, income doesn’t explain the diversities of their nutritional status, either. Population dietary studies published for well over 50 years have shown that in developed countries, low income children and families don’t eat appreciably different nutrients from higher income families.
A review of 196 published epidemiological studies examining diet quality and socioeconomic status in industrialized societies, for example, found that while people eat foods of different pedigrees, there is little biologically meaningful difference in total calories, fats, milk, protein, fruits and vegetables, or macronutrient compositions in the diets of people of differing socioeconomic status. The authors cautioned that poorly controlled studies, purportedly finding poorer nutrition among low socioeconomic groups, typically focus on at-risk groups and are not reflective of the general population. The recently published Low Income Diet and Nutrition Survey (LIDNS) of low-income families in the UK, monitored by the National Diet and Nutrition Survey (NDNS) programme, also found little difference in overall nutrients consumed among socioeconomic groups. This nationally representative survey of 3,728 of the most deprived households in the UK and is the most comprehensive medical exams and dietary analyses of its kind.
Mortality and weight gain
 While decades of epidemiological and clinical studies have failed to support popular beliefs in the health benefits of weight loss, these beliefs continue unquestioned by the general public— few hear the evidence that could help them question their assumptions. Similarly, the fact that the natural weight gain that comes with aging might be healthful is just as unthinkable to consumers. Yet, as this study by Dr. Strandberg and colleagues found, weight gain in adulthood has been shown to reduce mortality in countless well-controlled studies the public never hears about.
While decades of epidemiological and clinical studies have failed to support popular beliefs in the health benefits of weight loss, these beliefs continue unquestioned by the general public— few hear the evidence that could help them question their assumptions. Similarly, the fact that the natural weight gain that comes with aging might be healthful is just as unthinkable to consumers. Yet, as this study by Dr. Strandberg and colleagues found, weight gain in adulthood has been shown to reduce mortality in countless well-controlled studies the public never hears about.
The Honolulu Heart Program is just one of those reporting this paradox. It followed 6,537 middle-age Japanese American men over six years and after adjusting for age, smoking status, alcohol consumption, physical activity, socioeconomic status, caloric intake and preexisting disease, all-cause mortality was statistically higher among those who lost as little as 2.6 kg, while lower among those who gained 2.5 kg or more.
The adult years are characterized by a gradual and persistent physiologic increase in body weight, leading researchers to suggest that this age-related natural phenomenon may be protective and a major force in human longevity. The typical American adult gains 3–5 kg per decade beyond the age of 20 years, which translates into about 10–15 kg [22-33 pounds] between the third to fifth decades. The clinical research of Dr. Andres found that the fewest deaths occurred in those whose weights increased as they aged. Given the protective, fertility, immunological and nurturing benefits of fat stores, it is not surprising that the preponderance of medical research has failed to support beliefs that midlife weight gain is harmful to healthy women and men. With age, fat cells have also been shown to become less metabolically active, lessening their role in diseases associated with aging like diabetes.
“It’s acceptable, possibly even highly beneficial, for normal, healthy adults to gain gradually about a pound a year beginning around age 40,” said Dr. Andres in Food & Nutrition Digest, “so that by the time they’re in their 60s they weigh about 20 pounds more than the Met Life tables would suggest.”
The possible healthfulness of natural weight gain with aging, however, is a paradoxical idea in popular media. People may never think to question their beliefs about the deadliness of fat and benefits of weight loss when they never hear anything different.
The importance of research finding seeming paradoxes is that it make us think, question and not be afraid to learn where the evidence might really take us.
© 2009 Sandy Szwarc




<< Home