JFS Special: Health marketing from the CDC

Our government’s National Center for Health Marketing hosted its second National Conference on Health Communication, Media and Marketing* this past week in Atlanta, Georgia. The most interesting and helpful aspects of this conference are the history of this relatively new agency, which is behind our government’s preventive health messages, and the sponsor of this conference, which reveals the level of credibility behind so much public health information.
This conference was presented by the National Center for Health Marketing (NCHM), a division of the Center for Disease Control and Prevention, along with the National Cancer Institute (NCI), and the National Public Health Information Coalition (NPHIC).
The NPHIC is a coalition of mostly state departments of health who work in partnership to deliver the CDC and other public health messages of disease risks, in order to provide the necessary link to state and federal programs trying to incentivize the adoption of healthy lifestyle behaviors. Its mission statement states its intent “is to make public health public.”
The NCI, in addition to funding cancer and obesity research and running the National Center of Complementary and Alternative Medicine, supports a number of government obesity-related diet and physical activity programs, including the 5-A Day for Better Health program. As the clinical evidence continues to fail to support claims that any special diet or that fruits and vegetables prevent cancers, the NCI has had to work harder to market its message. Magical fruits, a few posts: here, here, here, here and here.
The government’s war on obesity depends on convincing the public that obesity is deadly and, hence, in need of its public health programs. The public health messages linking obesity with cancers have been so concerted, there are still people, even medical professionals, who believe obesity raises risks for cancers... few have heard that even the government’s own data disproves this belief. That’s called effective marketing.

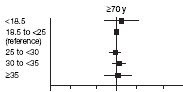 For instance, when senior CDC research scientists at the National Center for Health Statistics (NCHS) published the results of thirty years of mortality data from the National Health and Nutrition Examination Surveys (NHANES) and U.S. vital statistics, they found “little or no association of excess all-cancer mortality with any of the BMI categories. None of the estimates of excess deaths was statistically significantly different [from null].”
For instance, when senior CDC research scientists at the National Center for Health Statistics (NCHS) published the results of thirty years of mortality data from the National Health and Nutrition Examination Surveys (NHANES) and U.S. vital statistics, they found “little or no association of excess all-cancer mortality with any of the BMI categories. None of the estimates of excess deaths was statistically significantly different [from null].”
The government’s own health statistics threaten the CDC’s obesity-related diet and physical activity policies. Which brings us to the National Center for Health Marketing...
Retrospective
In 2005, these same research scientists from inside the CDC’s National Center for Health Statistics nearly brought down the government’s entire war on obesity — begun by their own CDC director, Julie Gerberding, and then Secretary of Health and Human Service (HHS), Tommy Thompson — when they published data exposing that it had all been a scandalously exaggerated and fabricated scare campaign. There weren’t 400,000 Americans dying each year of obesity, sedentary behaviors or poor diets, as was being claimed. The ‘obesity crisis’ had been derived from poor data with such flagrant methodological flaws, they showed, the computer modeling hadn’t even accounted for aging, the single biggest risk factor for death.
Instead of being deadly, ‘obesity’ (BMIs 30 to <35) was associated with a 24% lower risk for premature death than those of ‘normal’ weight, factoring for smoking. Yes, the researchers had accounted for smoking, as well as chronic diseases and preexisting health problems and cancer, involuntary weight loss and long-term obesity. Since age is the biggest risk factor for death, even the most ‘morbidly obese’ seniors with BMIs >35 were associated with a mere untenable 12-17% increased risk — still nowhere near those of thin people with 50-69% higher risks. Rather than 65% of Americans being accused of being “too fat” and risking early graves, it turns out that most fat people may actually outlive those of ‘normal’ weight. The “obesity crisis” isn’t nearly as dire as the HHS was messaging. But few of the public ever got this information. To this day.
Immediately after the release of this potentially devastating study in the Journal of the American Medical Association, obesity stakeholders from Harvard School of Public Health, the American Cancer Society, American Heart Association and Dr. Gerberding of the CDC, quickly held press conferences to, as Dr. Gerberding said, “translate our science more effectively so that we avoid this kind of communication in the future.”
As Dr. Gerberding told the media in a briefing on June 2, 2005, they were there to “straighten this out” and explain “the confusion” about the relationship between obesity and health events. [The HCHS scientists and authors of the study were nowhere in sight.] Citing an obesity epidemic, she said: “We know that obesity and overweight are important health threats.” She repeated the claims:
 People who are obese experience an increased rate of hypertension, diabetes, renal failure. They're at increased risk for cancers, including colon cancer, post-menopausal breast cancer, gall bladder cancer and uterine cancer. People who are obese and overweight have an increased risk of arthritis and mobility problems. People have sleep disturbances and breathing problems. Another very scary fact for children — Type II Diabetes, which used to be known as adult onset diabetes, is now increasingly being diagnosed and adding to the cardiovascular risk profile of our children. We have many children now who are not only overweight, but they also have high blood pressure, lipid abnormalities, and diabetes — all of the factors that increase the risk among adults for cardiovascular disease and stroke. We also know that obesity is linked to problems with child bearing, premature birth, learning disabilities, and other adverse outcomes for infants...
People who are obese experience an increased rate of hypertension, diabetes, renal failure. They're at increased risk for cancers, including colon cancer, post-menopausal breast cancer, gall bladder cancer and uterine cancer. People who are obese and overweight have an increased risk of arthritis and mobility problems. People have sleep disturbances and breathing problems. Another very scary fact for children — Type II Diabetes, which used to be known as adult onset diabetes, is now increasingly being diagnosed and adding to the cardiovascular risk profile of our children. We have many children now who are not only overweight, but they also have high blood pressure, lipid abnormalities, and diabetes — all of the factors that increase the risk among adults for cardiovascular disease and stroke. We also know that obesity is linked to problems with child bearing, premature birth, learning disabilities, and other adverse outcomes for infants...
CDC is taking a number of actions, but our most important action starts with the science. And, again, today, is the Institute of Medicine [2005] report on methods to estimate the association of obesity and death was released... I think it is a very beautiful summary, not only of the state of the science, but a roadmap for some of the things that we as an agency need to do to improve our science and our communication about these important health threats, and we are taking it seriously...
 It was at this press conference where most of the public first learned the CDC had been completely restructured, to create “the new CDC,” and of the newly-created National Center for Health Marketing. “At the new CDC, we are engaging the entire agency in the development of our strategies around obesity,” said Dr. Gerberding. About 15 CDC divisions and programs currently conduct overweight and obesity-related public health activities, she said. They all “came together to create what we're calling trailblazer goals for obesity,” which will enable them to “capitalize on CDC’s deep experience in population-based prevention efforts with schools and worksites, the communications and marketing fields, and the nation’s public health system.” She said these goals will “engage them collaboratively up front in tackling this very, very important health problem.”
It was at this press conference where most of the public first learned the CDC had been completely restructured, to create “the new CDC,” and of the newly-created National Center for Health Marketing. “At the new CDC, we are engaging the entire agency in the development of our strategies around obesity,” said Dr. Gerberding. About 15 CDC divisions and programs currently conduct overweight and obesity-related public health activities, she said. They all “came together to create what we're calling trailblazer goals for obesity,” which will enable them to “capitalize on CDC’s deep experience in population-based prevention efforts with schools and worksites, the communications and marketing fields, and the nation’s public health system.” She said these goals will “engage them collaboratively up front in tackling this very, very important health problem.”
Dr. Gerberding said:
Our National Center for Health Marketing is the place where we will be able to apply state of the art communications strategies so that we not only avoid confusing the public but also we use the very best science and the very best methods available to help people get the information they need to make healthy choices about diet and exercise and other preventable causes of ill health.
This CDC reorganization reportedly came from recommendation from her “Futures Initiative” obesity trailblazers, a group of more than 500 unnamed individuals and organizations from outside the CDC, described as partners, customers, decision-makers and stakeholders in healthy lifestyles and the CDC’s nutrition and physical activity initiatives. As Dr. Gerberding explained in a letter dated April 21, 2005, the restructuring was made official that day when “Congress accepted the CDC’s new strategic orientation.” With about 15,000 workers at the CDC and a budget of approximately $8 billion, she said the new structure will better align the CDC to achieve its goals:
The four new coordinating centers include the Coordinating Center for Environmental Health and Injury Prevention, the Coordinating Center for Health Promotion, the Coordinating Center for Infectious Diseases, and the Coordinating Center for Health Information and Services. In addition, CDC has added two new centers, the National Center for Public Health Informatics and the National Center for Health Marketing, to provide the science we need to create usable information that people need to make sound health decisions...
At a 2004 board meeting discussing the Futures Initiative, Dr. Edward Sondick, director of the NCHS, said that the bottom line is the NCHS was to be placed within the Coordinating Center for Health Information and Service, along with the National Center for Health Marketing and the National Center for Public Health Informatics. In other words, the NCHS (and its problematic science) was put behind several layers of political firewalls. Thereafter, all communications to the public would come through CDC communications and marketing departments. The CDC directors would have first access to NCHS data before it is released to the public to ensure that the scientific data was released as “actionable” points based on the government’s Healthy People goals. Concerns were raised by the NCHS board that its mission as a neutral federal research and statistical agency would be compromised.
You may remember that this restructuring resulted in a mass exodus of the top CDC scientists during 2004-2006 who were concerned with the honesty and integrity of science and the information reaching the public. By the end of 2006, in addition to more than a dozen leading scientists, all but two of the directors of CDC's eight primary scientific centers had left. As the Atlanta Journal-Constitution reported:
Trust issues range from a general lack of confidence that CDC's leadership will "do the right thing" when faced with political pressure from Washington; to questions of whether the reorganization was motivated more by a desire for control and power than designed to fix anything that was broken; to a belief that official staff communications are designed more to burnish a public relations image than give employees the unvarnished truth...
Current events
Coming back to the National Center for Health Marketing, according to its website, it’s mission is to protect and promote the public’s health through collaborative and innovative health marketing programs, products and services. Last week’s conference on Health Communication, Media and Marketing discussed strategies for delivering the government’s public preventive health and healthy lifestyles messaging. The conference was sponsored by Care2.com, Inc., a healthy diet and lifestyle information online portal.
 Nothing better exemplifies the degree that unsound science and alternative modalities have become inherent in preventive health and wellness, and popular beliefs that ‘healthy’ eating and lifestyles can prevent cancer, chronic diseases of aging, and obesity, than the sole sponsor of this program and its partners. Remember, this company was chosen by the CDC in its judgment, as part of its purportedly science-based public health messaging:
Nothing better exemplifies the degree that unsound science and alternative modalities have become inherent in preventive health and wellness, and popular beliefs that ‘healthy’ eating and lifestyles can prevent cancer, chronic diseases of aging, and obesity, than the sole sponsor of this program and its partners. Remember, this company was chosen by the CDC in its judgment, as part of its purportedly science-based public health messaging:
Going to its website on Monday, for example, the front page on Green Living offered articles on the raw food diet, do’s and don’ts of feng shui offices, green hair removal, ‘chemical dangers’ in car seats, healing foods: smoothies, quantum spirituality, five alternative heart tonics, gluten-free recipes, cilantro’s ability to remove heavy metals, and your Deepak Chopra quote of the day.
Its Health and Wellness page had 12 superfood herbs and spices, the new green diet, healing foods, a link to ten foods to fight aging and keep you young and face-saving foods, ayurvedic sinus solutions, rhodiola rosea for epic strength, agave to prevent diabetes and insulin deficiency and resistance, the Bach flower remedy olive, vitamin D3’s role in metabolic syndrome, and cinnamon to prevent and treat diabetes.
You get the idea. It really brought home the concerns mentioned by those exiting CDC scientists and directors; such as Dr. David Sencer who wrote about the erosion of the scientific base; Dr. Stephen Ostroff, former deputy director of CDC's National Center for Infectious Diseases, who worried that a lot of the CDC decision-making and resources were being moved away from the former scientific underpinnings of the agency; and Dr. Harold Margolis who said the new CDC shifts away from letting science drive programs.
It has never been more important for us to look critically at health information we read or hear, even when it comes from the government and other stakeholders, and no matter how well it’s marketed.
© 2008 Sandy Szwarc. All rights reserved.
* Second National Conference on Health Communication, Media and Marketing, 2008 Innovations in health communications, marketing and media — new media technologies and computer simulation training programs, using virtual worlds and avatars for changing behaviors, social marketing, web tracking, using text messaging and mobile technology in marketing campaigns for social change, polling and focus groups, and how to influence attitudes toward policy. Reducing health disparities — health literacy, reaching minority and low-income populations, communicating about HIV/AIDS, second-hand smoke marketing to children, church-based marketing of diets to African-Americans, and social marketing of Hepatitis B awareness among Asians in NYC. Disseminating public health program and information — media coverage and messaging; branded media campaigns such as 5 A Day; newspaper and wire services response to press releases; messaging to change behaviors; communicating threat of climate change; developing social marketing campaigns; using partnerships; designing multi-media campaigns on childhood obesity, colonoscopies, and HPV; communicating unhealthy eating, dietary fats, obesity and chronic disease risks; and using partnerships to raise awareness of heart disease in women. Getting the public to adopt healthy behaviors — health promotion campaigns and building partnerships, targeting women, second-hand smoke media campaigns and anti-smoking messaging, building public will, use of images that illicit fear and anxiety about obesity to help heighten perceptions of risk and change behaviors, online media and strategies for impacting health-information seeking behaviors, and writing success stories to build support for public health programs. The program offered talks on how to more effectively deliver public health messages, such as:
The program offered talks on how to more effectively deliver public health messages, such as:




<< Home